- Clinical Technology
- Adult Immunization
- Hepatology
- Pediatric Immunization
- Screening
- Psychiatry
- Allergy
- Women's Health
- Cardiology
- Pediatrics
- Dermatology
- Endocrinology
- Pain Management
- Gastroenterology
- Infectious Disease
- Obesity Medicine
- Rheumatology
- Nephrology
- Neurology
- Pulmonology
Acute MI With Long-Standing AIDS: A Perfect Storm of Risk Factors for Premature Coronary Artery Disease
The patient is a 54-year-old man, a native of Poland who has lived in the United States for many years. A diagnosis of AIDS was made in 1994, when Hodgkin disease (nodular sclerosing Hodgkin lymphoma) was found in an enlarged cervical lymph node and he tested positive for HIV during his workup.
The patient is a 54-year-old man, a native of Poland who has lived in the United States for many years. A diagnosis of AIDS was made in 1994, when Hodgkin disease (nodular sclerosing Hodgkin lymphoma) was found in an enlarged cervical lymph node and he tested positive for HIV during his workup. His lymphoma was treated successfully with ABVD (a chemotherapeutic regimen comprising doxorubicin [Adriamycin], bleomycin, vinblastine, and dacarbazine) and mediastinal radiation therapy. Now, 15 years later, he presents to the emergency department for evaluation of a new onset of chest pain.
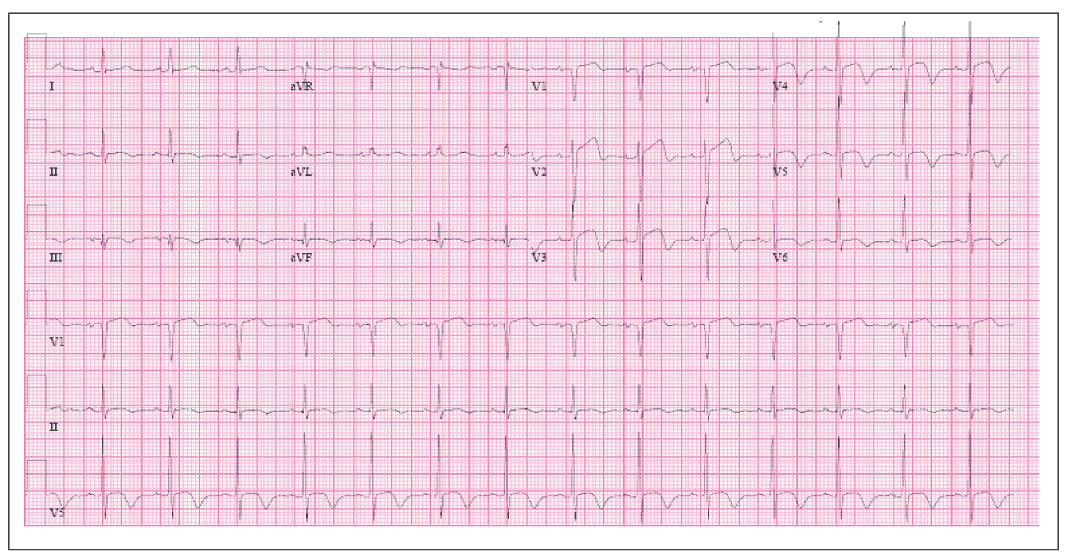
Figure. An ECG showing ST-segment changes consistent with myocardial infarction.
One day before admission, the patient awoke with fever (self-reported body temperature of 38.3°C [100.9°F]), cough productive of white blood-tinged sputum, mild pleuritic chest pain, and chest pressure associated with some shortness of breath. In the emergency room, his ECG tracing showed ST elevations (Figure); his initial troponin I level was 1.4 ng/mL (normal, 0.01 to 0.04), and a bedside echocardiogram revealed apical and septal hypokinesis.
The patient’s medical history was significant for a nadir CD4+ cell count of 20/µL in 1994. After completing mediastinal radiation therapy and chemotherapy, and subsequently beginning antiretroviral therapy with indinavir, stavudine, and lamivudine, his CD4+ cell count rose to a maximum of 250/µL and remained in that range for several years. Radiation therapy–associated hypothyroidism developed, and he is receiving low-dose thyroid hormone replacement therapy. He also presented with chemotherapy-associated polycythemia vera, which has been treated with phlebotomy on an as-needed basis. The patient has had no opportunistic illnesses and has been 100% adherent to his antiretroviral regimen. Both his blood pressure and cholesterol levels had been slightly elevated recently. He was taking hydrochlorothiazide and trying to modify his diet.
A review of systems revealed 6 months of a chronic cough and 2-pillow orthopnea over the same period. He has noted no decrease in his exercise tolerance over that 6-month period, reporting he is able to climb more than 5 flights of stairs and walk long distances with no shortness of breath. He uses cocaine approximately monthly and stated that his last use was 10 days before admission. Although he drinks a half pint of vodka daily, his responses to the CAGE questionnaire were entirely negative. He had smoked about 1 pack of cigarettes daily since adolescence, with a total 40-pack-year history, but he had quit about 6 months ago. The patient’s family history is notable for a brother, aged 56 years, who had had a myocardial infarction (MI); his father who died of heart disease at age 91; and his mother who died of heart disease at age 66. His current medications include a fixed-dose combination of efavirenz/tenofovir/emtricitabine, along with levothyroxine and hydrochlorothiazide.
On physical examination in the emergency department, he was comfortable sitting up on a stretcher, with body temperature of 36.7°C (98.1°F), heart rate of 87 beats per minute and regular, blood pressure of 109/66 mm Hg, weight of 70 kg (154 lb). Oxygen saturation on room air was 99%.
The patient had marked facial and limb lipoatrophy but no abdominal fat accumulation or dorsocervical fat pad. There was no thrush or cervical adenopathy noted. His chest was clear to auscultation, and although heart sounds were distant, there were no rubs, murmurs, or gallops. His jugular venous pressure was elevated 5 cm above the sternal angle. Bowel sounds were normal, and the abdomen was soft, flat, and without hepatosplenomegaly. His extremities were remarkable for prominent veins and decreased subcutaneous fat; there was no edema or cyanosis. Lower extremity pulses were symmetrical and palpable.
The patient’s initial laboratory test results were as follows:
• White blood cell count, 9400/µL (normal, 3400 to 11,200), with 68% neutrophils; hemoglobin level, 16.6 g/dL (normal, 11.7 to 16.0); platelet count 167,000/µL (normal, 150,000 to 450,000).
• Sodium, 138 mEq/L (normal, 136 to 144); potassium, 3.1 mEq/L (normal, 3.6 to 5.1); chloride, 103 mEq/L (normal, 101 to 111); bicarbonate, 24 mEq/L (normal, 22 to 32); blood urea nitrogen, 21 mg/dL (normal, 5 to 25); creatinine, 1.1 mg/dL (normal, 0.5 to 1.5); glucose, 106 mg/dL (normal, 70 to 105); calcium, 8.9 mg/dL (normal, 8.5 to 10.5); magnesium, 1.9 mEq/L (normal, 1.5 to 1.9).
• Transaminase and bilirubin levels were within normal limits.
• C-reactive protein level was 10.53 mg/dL (within normal range).
• Total cholesterol, 193 mg/dL (desirable, less than 200); high-density lipoprotein (HDL) cholesterol, 42 mg/dL (desirable, greater than 40); low-density lipoprotein (LDL) cholesterol (calculated), 139 mg/dL (desirable, less than 100); triglycerides, 62 mg/dL (desirable, less than 150).
• Creatine kinase, 500 U/L (normal, 46 to 295).
• Troponin I level peaked at 1.93 ng/mL (normal, 0.01 to 0.04).
• B-type natriuretic peptide, 458 pg/mL (normal, less than 100).
• Thyroid-stimulating hormone, 0.28 mU/L ( normal, 0.34 to 5.6).
• Urine drug screen positive for cocaine.
No infiltrates or cardiopulmonary pathology was seen on the initial chest radiograph. An echocardiogram obtained in the cardiac care unit on the day of admission showed apical thrombus and severe hypokinesis of the apical anterior and inferior walls, with an ejection fraction of 40% to 45% (expected range, 55% to 75%). A subsequent cardiac study with contrast the next day showed no evidence of thrombus, with an ejection fraction of 55%. A cardiac MRI scan obtained 5 days after admission showed an ejection fraction of 54% and evidence of transmural MI involving 75% to 100% of the basal ventricular wall, 50% to 75% of the mid and distal inferior wall, and 25% to 50% of the basal inferoseptum. A subendocardial infarction of the inferoseptum was also noted.
The results of a cardiac catheterization revealed severe 3-vessel disease with proximal left anterior descending coronary artery stenosis of 90%, mid-right coronary artery stenosis of 100%, and left main coronary artery stenosis of 50%.
The patient initially received anticoagulation therapy, aspirin, atorvastatin, and metoprolol; the latter was held when his history of recent cocaine use was revealed. Lisinopril, thiamine, and folate were added, and his current antiretroviral regimen and levothyroxime therapy were continued. Hydrochlorothiazide was discontinued.
The patient underwent a saphenous vein coronary artery bypass graft (CABG) of both his anterior descending artery and his obtuse marginal circumflex artery on day 6 of his hospitalization.
Although he had some persistent dyspnea and a single episode of oxygen desaturation during his recovery, an evaluation for pulmonary embolus and pneumonia were negative. The patient was discharged on postoperative day 8 to a nursing facility for a brief period of rehabilitation. His cardiac status remained stable as of the last follow-up, 8 weeks after the event.
THE CLINICAL CHALLENGE
The clinical challenge with this patient, as with many like him, is to make an accurate assessment of the risks for non–AIDS-defining illnesses and to follow up with appropriate interventions as needed. Accelerated or premature coronary artery disease has been defined as the development of coronary atherosclerosis before age 55 in men and age 65 in women.1 In this patient, it seemed his severe coronary artery disease was essentially clinically silent until he presented with atypical chest pain and a large transmural MI.
Given the list of risk factors for cardiovascular disease, some of which we are still learning to assess, this patient’s course represents a concurrence of various risk factors that resulted in a major cardiovascular event. I will review some of his individual risks for cardiovascular disease and discuss the possible contributing role of HIV infection and its treatment. Newer methods for evaluating subclinical coronary artery disease will also be discussed.
CARDIOVASCULAR EVENTS
The first large study to evaluate cardiovascular events and antiretroviral therapy, results of which were published in 2003, was a retrospective review of more than 36,000 patients within the Veterans Administration who had a median antiretroviral exposure of 15 months.2 During the short term, the study investigators found no increased rates of cardiovascular or cerebrovascular deaths or related hospital admissions and found that the benefit of antiretroviral therapy was not offset by increased rates of MI or cerebrovascular disease. This was reassuring to most clinicians at first, but subsequently, there has been some concern, despite the huge sample size, that monitoring disease progression during a short interval may not have captured all the vascular events.
A concurrent study, results of which were published in 2002, evaluated more than 5000 HIV-positive outpatients at 9 US clinics and showed the frequency of MI increased significantly in patients treated with a protease inhibitor (PI)-containing regimen (odds ratio [OR], 7.1; 95% confidence interval [CI] 1.6 to 44.3).3 More recently, an analysis of more than 18,603 HIV-positive patients from the International Network for Strategic Initiatives in Global HIV Trials (INSIGHT) and the HIV Outpatient Study (HOPS) cohorts treated for a median of 3.5 years showed only a slight increase in the risk of MI associated with PI-based treatment (hazard ratio, 1.19; 95% CI, 1.01 to 1.40).4 The authors in this study concluded that the overall benefits of PI- and NNRTI-based antiretroviral regimens in reducing mortality significantly outweigh any risks of atherosclerotic disease in the short term. They further stated that modification of traditional cardiac risk factors may be more beneficial than attempting to reduce risk through changing a patient’s antiretroviral therapy.
Epidemiologically, the impact of traditional risk factors for cardiovascular disease compared with the impact of HIV or its treatment on mortality associated with cardiovascular disease has been difficult to disentangle. The survival advantage conferred by highly active antiretroviral therapy may confound the ability to identify cardiovascular toxicities related to HIV treatment. HIV infection itself may contribute to cardiovascular risk in certain patients.
The most comprehensive assessment of cardiovascular events in HIV-infected patients to date has been generated from the Data Collection of Adverse Events of Anti-HIV Drugs (D:A:D) study. This study was initiated in 1999 as a prospective observational cohort of HIV-infected patients at 11 international sites. The primary outcome of this study was MI. In 2007, an analysis of the data from more than 23,000 HIV-infected persons was published.5 Median age of the patients studied was 39, and approximately one-quarter were women. The investigators found that the traditional risk factors (eg, smoking; hypertension; elevated total cholesterol, LDL cholesterol, and triglyceride levels; diabetes; and family history of cardiovascular disease) are associated with MI in this population, but they also assessed the relationship of cardiovascular outcomes to antiretroviral therapy.
Through February 2005, 345 fatal and nonfatal MIs were observed for an overall incidence rate of approximately 3.7 per 1000 person-years. The median exposure to antiretroviral therapy was 6.9 years, and more than 90% of patients had some exposure to antiretroviral treatment. Overall, the risk of MI was found to increase with longer exposure to antiretroviral therapy, with a nearly linear increase of 26% in the rate of MI per year of exposure to antiretroviral therapy during the first 4 to 6 years of use. The relative rate per year of exposure to a PI-based regimen after adjustment for demographic factors, body mass index, family history, and smoking was 1.16. When lipid data were added to the adjusted model, although the estimate of MI risk with increasing exposure to PIs decreased, the effect was not abrogated completely, suggesting that not all of the PI effect is attributable to lipid abnormalities alone. MI was not associated with control of HIV infection or CD4 count.
The D:A:D study has been ongoing and now includes 33,347 HIV-infected persons, and additional analyses were recently presented. As of October 2007, a total of 2192 deaths had occurred in the cohort since the start of the study. Cardiovascular disease accounted for 11% of these deaths.6
SUBCLINICAL CORONARY ARTERY DISEASE
Although risk factor assessment based on epidemiological studies may be useful in targeting interventions to decrease overall risk, noninvasive imaging to ascertain true arterial disease has been validated in predicting cardiovascular events using 2 techniques: B-mode ultrasonography for measuring carotid intima-media thickness (cIMT)7 and electron beam tomography (EBT) for assessing coronary artery calcification.8,9 Recently published data have shown that these techniques can be applied to HIV-infected persons.
In an analysis of coronary artery calcification using EBT in 947 men in the Multicenter AIDS Cohort Study (MACS) cohort, not surprisingly, increasing age was most strongly associated with both the prevalence and extent of coronary artery calcification for all the study groups (HIV-negative, HIV-positive antiretroviral-naive, and HIV-positive receiving treatment).10 After adjustment for traditional risk factors, both HIV infection and long-term use of antiretroviral therapy increased the odds for the presence of coronary artery calcification, which is distinct from the extent of calcification. Although the prevalence of calcification was marginally increased among long-term antiretroviral-treated patients, the extent of the coronary artery calcification seen was actually significantly less among patients receiving antiretroviral therapy than among their HIV-seronegative controls. Although this MACS report suggests that HIV and antiretroviral therapy are risks factors for the development of coronary artery calcification, more antiretroviral-treated men were also receiving lipid-lowering therapy (40%) than HIV-negative men (20%). This may help to explain the discrepancies in the extent of coronary artery calcification between the HIV-positive men receiving antiretroviral treatment and the HIV-negative men.
Another study looked at both types of imaging in 314 HIV-infected men and women with metabolic syndrome or without metabolic syndrome.11 These investigators found both groups were equally likely to have a high internal cIMT score (greater than 1.0 mm), and in a multivariate analysis adjusted for demographics and smoking, participants with metabolic syndrome were more likely to have an abnormal common cIMT measurement (OR, 2.9; P = .020) and detectable coronary artery calcification scores (OR 4.9; P < .0001) but not a higher internal cIMT measurement. It appears the metabolic syndrome may behave the same way in HIV-infected persons as in uninfected persons and may lead to accelerated atherosclerosis.
RISK FACTOR ASSESSMENT
Certain traditional risk factors for cardiovascular events occur more frequently in both treated and untreated HIV-positive persons. Lower HDL cholesterol levels, higher triglyceride levels, increased visceral adiposity, and smoking all have been reported to be more prevalent in the HIV-infected population than in population-based cohorts without coronary artery disease.12 The Framingham risk calculator (available at http://hp2010.nhlbihin.net/atpiii/calculator.asp?usertype=prof) can be useful for evaluating patients for some traditional risk factors and can help categorize risk and level of intervention for modifiable risk factors.
Recent data from the Fat Redistribution and Metabolic Change in HIV Infection 2 (FRAM 2) study suggest that HIV infection itself may be as significant a risk factor for a subsequent major cardiac event as many of the traditional risk factors. Assessment of risk was determined by degree of carotid intima-media thickness in a cross-sectional study of 433 HIV-infected and 5749 control HIV-negative persons without previous cardiac events. Even after adjustment for demographic characteristics and traditional risk factors for cardiovascular disease (eg, smoking, diabetes, hypertension, and dyslipidemia), HIV infection remained an independent risk factor similar in magnitude to that of traditional risk factors, including smoking, diabetes, and male sex.13
COCAINE AND CORONARY ARTERY DISEASE
Cocaine-associated cardiovascular events, often thought to be related to coronary artery vasospasm, have been documented in the literature for a number of years.14 In vitro, cocaine appears to cause endothelial cell defects that increase endothelial adhesion molecule production and set the stage for accelerated atherosclerosis.15 The results from a study of cocaine use in 224 patients in Baltimore demonstrated that subclinical coronary artery disease as assessed by the presence of coronary artery calcification was most prevalent in the proportion of patients who were both HIV-infected and cocaine users.16 A follow-up study using CT coronary angiography found that the prevalence of significant stenosis (greater than 50%) was 42% among those who had used cocaine for more than 15 years and had received antiretroviral therapy for at least 6 months.17 Each factor was independently associated with the presence of significant coronary stenosis.
LIPODYSTROPHY AND INFLAMMATORY BIOMARKERS
Studies of lipodystrophy in HIV-infected patients receiving treatment have found that according to Framingham criteria, the 10-year risk of cardiovascular disease was higher in these patients than in both controls and HIV-infected patients without lipodystrophy.18,19 Of interest, the highest risk calculation was seen in patients with primary lipoatrophy rather than lipoaccumulation.18 The strongest association with lipodystrophy is most likely the metabolic syndrome, a known risk factor for progressive atherosclerosis.19
Biomarkers, especially those associated with vascular disease, such as high-sensitivity C-reactive protein and proinflammatory cytokines, along with endothelial activation markers (soluble intercellular and vascular cell adhesion molecules and von Willebrand factor), were associated with HIV positivity in a study of 182 HIV-infected participants.20 In this study, there was no association between HIV positivity and lipoatrophy. Treatment-naive persons demonstrated enhanced levels of endothelial activation markers, bolstering again the argument that HIV infection itself, possibly through mechanisms of inflammation, is a substantial risk factor for the development of cardiovascular disease.
Genomics has become more prominent in developing predictive models for many disease states, and newly identified loci have been associated with development of coronary atherosclerosis. The chromosome 9p21.3 locus contains genes for cyclin-dependent kinase inhibitors, which affect cell proliferation, aging, and apoptosis21-all of which are likely to be important in the pathogenesis of coronary artery disease.
CONCLUSION
In addition to traditional risk factors for coronary artery disease (eg, older age, male sex, family history), this patient’s elevated LDL cholesterol level, cocaine use, lipoatrophy, smoking history, and possibly his long-standing HIV infection itself added up to more than the usual risk factors for coronary artery disease. Mediastinal radiation therapy, which has been reported to be associated with coronary events,22 probably added another level of risk. Polycythemia, which, if uncontrolled, could also predispose to reocclusion of bypass grafts. The risk of subsequent occlusion of another native vessel after a CABG was higher for HIV-infected persons than for uninfected case-matched controls in one small series.23 Although the patient described in this clinical challenge found a surgical harbor in this perfect storm of cardiovascular risk factors, it may be only temporary.
References:
References1. Person AF, Patterson C. Therapeutic options for premature coronary artery disease. Curr Treat Options Cardiovasc Med. 2008;10:294-303.
2. Bozzette SA, Ake CF, Tam HK, et al. Cardiovascular and cerebrovascular events in patients treated for human immunodeficiency virus infection. N Engl J Med. 2003;348:702-710.
3. Holmberg SD, Moorman AC, Williamson JM, et al; HIV Outpatient Study (HOPS) Investigators. Protease inhibitors and cardiovascular outcomes in patients with HIV-1. Lancet. 2002;360:1747-1748.
4. Kwong GP, Ghani AC, Rode RA, et al. Comparison of the risks of atherosclerotic events versus death from other causes associated with antiretroviral use. AIDS. 2006;20:1941-1950.
5. DAD Study Group, Friis-Møler N, Reiss P, Sabin CA, et al. Class of antiretroviral drugs and the risk of myocardial infarction. N Engl J Med. 2007;356:1723-1735.
6. Smith C; D:A:D Study Group. Association between modifiable and non-modifiable risk factors and specific causes of death in the HAART era: the data collection on adverse events of anti-HIV drugs study. 16th Conference on Retroviruses and Opportunistic Infections; February 8-11, 2009; Montreal. Abstract 145.
7. O’Leary DH, Polak JF. Intima-media thickness: a tool for atherosclerosis imaging and event prediction. Am J Cardiol. 2002;90:18L-21L.
8. Greenland P, Bonow RO, Brundage BH, et al. ACCF/AHA 2007 clinical expert consensus document on coronary artery calcium scoring by computed tomography in global cardiovascular risk assessment and in evaluation of patients with chest pain: a report of the American College of Cardiology Foundation Clinical Expert Consensus Task Force (ACCF/AHA Writing Committee to Update the 2000 Expert Consensus Document on Electron Beam Computed Tomography) developed in collaboration with the Society of Atherosclerosis Imaging and Prevention with the Society of Cardiovascular Computed Tomography. J Am Coll Cardiol. 2007;49:378-402.
9. Agatston AS, Janowitz WR, Hildner FJ, et al. Quantification of coronary artery calcium using ultrafast computed tomography. J Am Coll Cardiol. 1990;15:827-832.
10. Kinglsey LA, Cuervo-Rojas J, Muñoz A, et al. Subclinical coronary atherosclerosis, HIV infection and antiretroviral therapy: Multicenter AIDS Cohort Study. AIDS. 2008;22:1589-1599.
11. Mangili A, Jacobson DL, Gerrior J, et al. Metabolic syndrome and subclinical atherosclerosis in patients infected with HIV. Clin Infect Dis. 2007;44:1368-1374.
12. Savès M, Chêne G, Ducimetière P, et al; French WHO MONICA Project and the APROCO (ANRS EP11) Study Group. Risk factors for coronary heart disease in patients treated for human immunodeficiency virus infection compared with the general population. Clin Infect Dis. 2003;37:292-298.
13. Grunfeld C, Delaney J, Wanke C, et al. HIV infection is an independent risk factor for atherosclerosis similar in magnitude to traditional cardiovascular disease risk factors. 16th Conference on Retroviruses and Opportunistic Infections; February 8-11, 2009; Montreal. Abstract 146.
14. Dressler FA, Malekzadeh S, Roberts WC. Quantitative analysis of amounts of coronary arterial narrowing in cocaine addicts. Am J Cardiol. 1990;65:303-308.
15. Gan X, Zhang L, Berger O, et al. Cocaine enhances brain endothelial adhesion molecules and leukocyte migration. Clin Immunol. 1999;91:68-76.
16. Lai S, Lima JA, Lai H, et al. Human immunodeficiency virus 1 infection, cocaine and coronary calcification. Arch Intern Med. 2005;165:690-695.
17. Lai S, Fishman EK, Lai H, et al. Long-term cocaine use and antiretroviral therapy are associated with silent coronary artery disease in African Americans with HIV infection who have no cardiovascular symptoms. Clin Infect Dis. 2008;46:600-610.
18. Hadigan C, Meigs JB, Wilson PW, et al. Prediction of coronary heart disease risk in HIV-infected patients with fat redistribution. Clin Infect Dis. 2003;36:909-916.
19. Isomaa B, Almgren P, Tuomi T, et al. Cardiovascular morbidity and mortality associated with the metabolic syndrome. Diabetes Care. 2001;24:683-689.
20. Ross AC, Armentrout R, O’Riordan MA, et al. Endothelial activation markers are linked to HIV status and are independent of antiretroviral therapy and lipoatrophy. J Acquir Immune Defic Syndr. 2008;49:499-506.
21. McPherson R, Pertsemlidis A, Kavaslar N, et al: A common allele on chromosome 9 associated with coronary heart disease. Science. 2007;316:1488-1491.
22. Schulman HE, Korr KS, Myers TJ. Left internal thoracic artery graft occlusion following mediastinal radiation therapy. Chest. 1994;105:1881-1882.
23. Boccara F, Cohen A, Di Angelantonio E, et al. Coronary artery bypass graft in HIV-infected patients: a multicenter case control study. Curr HIV Res. 2008;6:59-64.
